*1:For the April-June quarter of 2020, the gross domestic product (GDP) decreased by 8.3% in real terms from the previous quarter, which is an annualized decrease of 29.3% (Source: Basic Policies for Novel Coronavirus Disease Control dated March 28, 2020 (revised on February 26, 2021) decided by the Novel Coronavirus Response Headquarters).
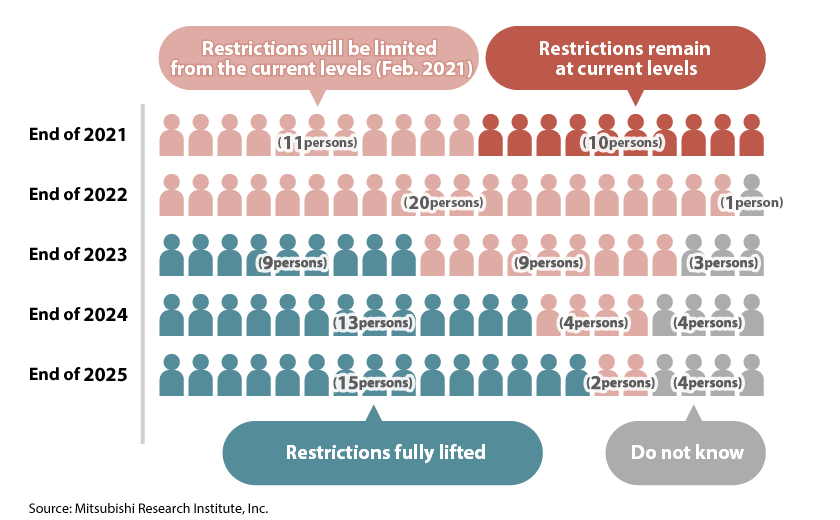
*2:Among experts in infectious disease with whom the MRI has connections, about 30 experts were requested to reply to a survey. They included those from the Expert Meeting on Novel Coronavirus Disease Control under the Cabinet Secretariat; the Advisory Board Meeting for COVID-19 measures of Ministry of Health, Labour and Welfare (MHLW); Infectious Disease Working Group Meeting of the Health Sciences Council, MHLW; and the Cluster Response Team of MHLW, and responses were obtained from 21 of them (February 21 to 28, 2021).
The specialized fields of the 21 experts who responded were basic medicine (microbiology/immunology): 2, clinical medicine (internal medicine): 4, social medicine (public health/hygienics): 11, and others (molecular biology, pediatrics): 2.
*3:The MHLW website “Instructions for the COVID-19 vaccination (Manufactured by Pfizer)”
https://www.mhlw.go.jp/stf/seisakunitsuite/bunya/vaccine_pfizer.html (accessed on March 3, 2021)
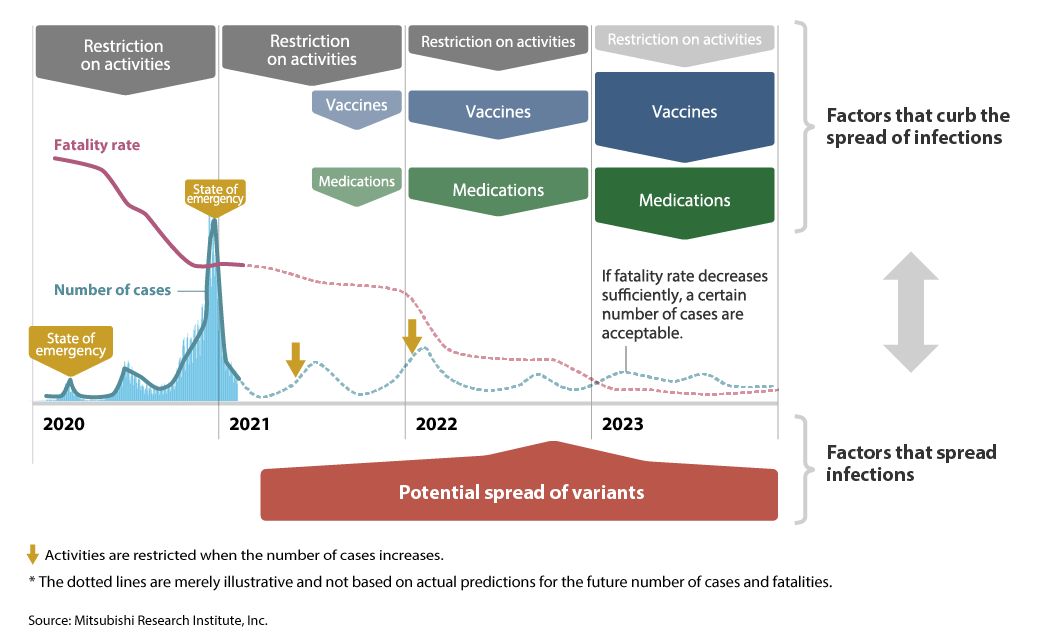
*4:The fatality rate was obtained by dividing the number of deaths by the number of infections (the number of PCR-positive cases).
The MHLW website “Coronavirus Disease 2019 (COVID-19) Situation in Japan (including the data published by the local governments on May 31)”
https://www.mhlw.go.jp/stf/newpage_11612.html (accessed on March 17, 2021)
The MHLW website “Coronavirus Disease 2019 (COVID-19) Situation in Japan (including the data published by the local governments on March 15)”
https://www.mhlw.go.jp/stf/newpage_17403.html (accessed on March 17, 2021)
*5:The Infectious Disease Working Group Meeting of the Health Sciences Council of MHLW (Document submitted by the National Institute of Infectious Diseases on January 15, 2021)
https://www.mhlw.go.jp/content/10906000/000720345.pdf (accessed on March 17, 2021)
*6:The MHLW website “Notice on COVID-19 vaccination”
https://www.mhlw.go.jp/stf/seisakunitsuite/bunya/0000121431_00218.html (accessed on March 3, 2021)
*7:The National Institute of Infectious Diseases “New variant of the novel coronavirus (SARS-CoV-2) that may have increased infectivity/transmissibility and different antigenicity (the 6th report)”
https://www.niid.go.jp/niid/ja/diseases/ka/corona-virus/2019-ncov/10169-covid19-35.html (accessed on March 3, 2021)
*8:In media reports, they are referred to as “the UK variant or the South African variant.” These are common names that are used as the variants were initially confirmed in the respective countries.